|
Many Gulf War veterans have experienced a variety of physical symptoms,
collectively called Gulf War illnesses. In response to veterans’
concerns, the Department of Defense established a task force in
June 1995 to investigate those incidents and circumstances related
to possible causes of these unexplained illnesses. The Office of
the Special Assistant assumed responsibility for these investigations
on November 12, 1996, and continues to gather information on environmental
and occupational exposures during the Gulf War and their possible
effects on the health of the troops who served there.
To inform the public about the progress
of this office, the Department of Defense publishes (on the Internet
and elsewhere) accounts related to the possible causes of illnesses
among Gulf War veterans, along with documentary evidence or personal
testimony used in compiling the accounts. The following is a summary
of the reports we have published concerning our investigations into
environmental and occupational exposures.
 |
We are all exposed to chemicals every day. |
We are all exposed to chemicals in
the air we breathe and in the food and water we consume every day.
Some of these chemicals are man-made while others occur in nature.
Someone living in a rural area will be exposed to different chemicals
than someone who lives in a large city. Proximity to farms and industries,
prevailing winds, and sources of food and water are some of the
variables that affect the types and levels of chemicals in our environment.
Furthermore, all environmental media can be affected; that is, air,
water and soil can become repositories for chemicals released on
a daily basis from human activities and natural actions. As a result,
we are exposed to chemical contaminants on a continuous basis in
our everyday lives.
 |
Chemical exposure varies depending on where
you live... |
Our occupations often expose us to
chemicals, too. A factory worker may be exposed to all the chemicals
used in the factory, more so to those specific chemicals he or she
works with every day. Occupational exposures can potentially be
more severe than other types of environmental exposures because
the concentrations of chemicals encountered in an occupational environment
tend to be much higher than in the ambient environment, and individual
workers are exposed to these higher levels of chemicals over longer
periods.
 |
...and where you work |
Several factors combine to determine
an exposure’s potential for causing illness: the toxicity of
the chemical, the concentration of the chemical, and the duration
of exposure are important factors for the potential for causing
illness. An individual’s susceptibility to the chemical adds
another variable.
Occupational exposures are usually
calculated for a 40-hour workweek, 50 weeks a year, over a 40-year
working life. Human health effects from chemical exposures are determined
from actual incidents experienced by people in occupations where
they are routinely exposed to toxic chemicals, or are estimated
based on studies involving animals in controlled laboratory environments.
 |
A factory worker is potentially exposed
to all the chemicals used in the factory. |
US military personnel who served in
the Gulf War were not only exposed to chemicals in the ambient environment;
they were also exposed to chemicals associated with their occupational
activities. For example, pesticides were widely used to control
insects, rodents, and other disease-carrying pests. These pesticides
were applied where veterans worked, ate, and slept. Some subgroups
of the general military population, that is, applicators who were
involved in the day-to-day handling and use of pesticides, and who
did not wear personal protective equipment, may have been exposed
to certain pesticides above levels considered safe for human health.
This is a concern because if improperly used, pesticides have the
potential to cause adverse health effects. That is, pesticides that
were used improperly may have created exposures above recommended
limits – for example, the use of some pesticides formulated
for use only in an outdoor environment were sometimes used indoors.
Such use could have resulted in overexposures.
 |
Pesticides were used extensively in the
Gulf to control sand flies and other disease-carrying insects. |
The Office of the Special Assistant
has investigated the potential for human health effects arising
as a result of exposure to pesticides and a number of other environmentally
and occupationally related factors experienced by some US military
personnel during the Gulf War. These investigations have resulted
in the preparation of environmental exposure reports that discuss
the issues and facts surrounding specific exposures. Some of these
reports also estimate the likelihood that long-term adverse health
effects could result. The reports are divided between environmentally
and occupationally related exposures. Environmentally related issues
included oil well fire smoke, particulate matter, and contaminated
water. Occupationally related issues included pesticides, chemical
agent resistant coating (CARC) paint, retrograde contaminated equipment,
and depleted uranium.
All of the environmental and occupational
related reports prepared by the Office of the Special Assistant
have been published on the Department of Defense’s GulfLINK
Web site and are briefly discussed in the following paragraphs.
 |
To many, oil well fires were the most obvious
threat to the health of our troops. |
Oil Well Fires
In response to the Iraqi’s occupation
of Kuwait, nearly 700,000 US troops were deployed during the Gulf
War in 1990 and 1991. In addition to the risk of sustaining combat
casualties, many of these troops were exposed to a number of toxic
substances from a variety of sources. The most visible source was
the smoke from hundreds of oil well fires that burned out of control
over a period of about nine months. Depending on their proximity
to the burning oil wells, veterans were exposed to varying levels
of petroleum combustion pollutants for hours to months in duration.
Non-documented reports by some veterans of various short-term, adverse
health symptoms occurred during the war. Some of these may have
been related to exposures to oil fire smoke. Air monitoring studies
and a review of records of reported adverse health effects did not
reveal a widespread short-term problem, but the possibility remained
that smoke exposures could cause diseases to develop in the future.
The results of the investigation into the potential health effects
of exposure to the smoke from the oil well fires in Kuwait is documented
in our Oil
Well Fires Environmental Exposure Report. Our report includes
a summary of the facts associated with this issue as well as the
results and findings of research conducted by other organizations.
Particulate Matter
 |
Particulate matter levels were often twice
that recommended for safeguarding health. |
The Oil Well Fires Environmental Exposure
Report identified several issues that required additional investigation
by us and further research by other organizations to resolve whether
exposure to contaminants from natural and man-made sources could
lead to long-term illness or explain any of the undiagnosed symptoms
reported by some Gulf War veterans. One area identified for further
investigation was the health effects associated with exposure to
particulate matter. The Particulate
Matter Environmental Exposure Report presents the results of
our investigation and discusses what we currently know about US
personnel exposures to particulate matter during the Gulf War.
 |
Some veterans voiced concerns that the water
supply may have contributed to their unexplained illness. |
Water Use
The rapid influx of Coalition forces into the Persian
Gulf region during the early stages of Operation Desert Shield taxed
the region's available potable water resources. Host nation and
commercial outlets were unable to provide sufficient supplies of
potable water to incoming troops. Water purification systems were
brought in by the United States to supply US forces with chlorinated
drinking water and water use policies were implemented in theater
with respect to non-potable water.
After the Gulf War, some veterans
became concerned about a possible relationship between water use
during the Gulf War and their illnesses. Anecdotal reports suggested
that some short-duration illnesses such as diarrhea and similar
gastrointestinal illnesses may have been triggered by contaminated,
over-chlorinated, or improperly stored drinking water, or by contaminated
water used to grow the local produce eaten by veterans. The Office
of the Special Assistant initiated the Water
Use investigation to determine if these individual episodes
could be linked to post-war illnesses reported by some veterans.
Pesticides
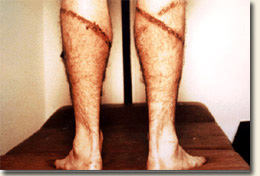 |
Flea and tick collars used by some US troops
caused skin irritation. |
Troops used pesticides during the
Gulf War for a number of purposes: on their skin and uniform to
repel insects; in area sprays and fogs to kill flying insects; in
pest strips and fly baits to attract and kill flying insects; and
as delousing agents applied to enemy prisoners of war to control
body lice. Pesticides used according to label directions (and with
the use of appropriate personal protective equipment) pose a minimal
health threat to most adults, but there are numerous reports of
health problems, in occupational settings, resulting from overexposure—either
through accident or misuse—to pesticides. The photo to the
right illustrates misuse of a pesticide product. In this case the
individual experienced a dermal reaction from wearing pet flea and
tick collars. The potential for health problems from pesticide overexposure
led some veterans and members of the medical and scientific communities
to express concern over the long-term health consequences of pesticide
use during the Gulf War. In response to these concerns, the Office
of the Special Assistant investigated pesticide use during the Gulf
War, and in March 2001, published the Pesticides
Environmental Exposure Report. Our report describes how pesticides
were used in the Gulf and describes what is known in the general
literature about health effects associated with exposures to pesticides.
In addition, the report presents what is known regarding the health
effects that may have been experienced by those who were exposed
to pesticides during their deployment to the Gulf.
 |
Much of the equipment arrived in the Gulf
with a green woodland camouflage scheme. |
Chemical Agent Resistant Coating
As part of the Operations Desert Shield
and Desert Storm deployment, the US shipped thousands of vehicles
and other equipment to the Persian Gulf. Much of the equipment had
the three-color woodland camouflage scheme designed for the European
theater, which would make it easy to spot in the barren desert environment.
Consequently, there was an operational requirement to repaint incoming
equipment with tan-colored urethane-based paint called chemical
agent resistant coating, or CARC, to provide desert camouflage protection.
 |
Coatings used in repainting operations contain
isocyanates, which in an occupational setting have shown to
cause respiratory problems. |
The military established a hand full
of painting operations in Saudi Arabia to paint the vehicles. Some
of these sites lacked the appropriate personal protective equipment
to assure safe spray painting operations. Due to the lack of adequate
personal protection, and a failure to adhere to applicable safety
and occupational health policies and procedures, a number of soldiers
directly involved in CARC painting may have suffered adverse health
effects, primarily respiratory effects from exposures to hexamethylene
diisocyanate (HDI) and solvents. Several spray painters at these
sites reported short-term symptoms, including coughing, eye and
throat irritation, skin rashes, headaches, and nausea. The Office
of the Special Assistant investigated CARC
to document its use, estimate to potential for exposure, and identify
the potential health issues associated with these exposures.
Retrograde Equipment
 |
Some are concerned they may have been exposed
to contaminants from equipment shipped back to the US. |
At the end of the Gulf War, US military
units began preparing equipment for redeployment back to their respective
peacetime installations. These retrograde operations saw large numbers
of vehicles and equipment assembled at sites where they were cleaned
and processed in accordance with strict protocols for materials
about to enter US air and sea ports. These protocols are meant to
prevent the spread of disease and protect US agricultural resources
from plant and animal pests and diseases that may be brought into
the country by contaminated equipment.
Some military and civilian personnel
who participated in processing the retrograde equipment are concerned
that they may have been exposed to battlefield or general environmental
contaminants that may have resulted in adverse health effects. In
response to these concerns, the Office of the Special Assistant
conducted the Retrograde
Equipment investigation to determine whether there were any
documented incidences of adverse health effects resulting from exposures
to this equipment.
 |
Some veterans expressed concern about the
chemical toxicity and radiological properties of DU and possible
health risks from its use. |
Depleted Uranium
The Gulf War was the arena for the
first battlefield use of armor-piercing munitions and reinforced
tank armor incorporating depleted uranium. This very dense metal
is a byproduct of the process by which natural uranium is enriched
to produce reactor fuel and nuclear weapons components. The leftover
uranium, 40% less radioactive than natural uranium, is called depleted
uranium, or DU. DU played a key role in US forces’ overwhelming
success during the Gulf War. The extreme density of the metal and
its self-sharpening properties make DU a formidable weapon. DU projectiles
slice through thicker, tougher armor at greater ranges than do other
high-velocity rounds. US forces also used DU to enhance their tanks’
armor protection. While DU’s combat debut showed the metal’s
clear superiority for both armor penetration and protection, its
chemical toxicity—common to all forms of uranium and similar
to other heavy metals such as lead and tungsten—and its low-level
radioactivity raised concerns about possible combat and non-combat
health risks of DU. An investigation into the use of DU
in the Gulf was conducted to determine whether DU posed an unacceptable
health risk to American forces and whether personnel had been adequately
trained to deal with this risk.
Focus on Current and Future
Deployments
Collectively the investigations to-date
into environmentally and occupationally related factors have further
demonstrated the Office of the Special Assistant’s intention
to leave no stone unturned in attempting to answer the question
of what is causing the unexplained illnesses reported by some Gulf
War veterans. While we have found no evidence of any environmental
factor that can be directly and solely attributed to any of the
illnesses reported by some veterans, we continue to pursue issues
that may have a bearing on this question. Currently our efforts
continue to focus on the health-related environmental issues not
only of the Gulf War but also on current and future deployments.
The ultimate goal is to insure that the concerns of veterans are
consistently answered for them by the Department of Defense through
consistent implementation of force health protection activities.
Additional Information Resources
The following web links provide additional
scientific and technical information related to the environmental
and occupational exposures that may have been experienced by our
troops during Operations Desert Shield and Desert Storm.
- Department of Health and Human Services, "Preventing
Asthma and Death from Diisocyanate Exposure," Department
of Health and Human Services (NIOSH) publication no. 96-111,
1996.
- RAND Corporation, A Review of the Scientific Literature
as it Pertains to Gulf War Illnesses, Vol. 6 – Oil
Well Fires.
- RAND Corporation, A Review of the Scientific Literature
as it Pertains to Gulf War Illnesses, Vol. 7 – Depleted
Uranium.
- RAND Corporation, A Review of the Scientific Literature
as it Pertains to Gulf War Illnesses, Vol. 8 – Pesticides
- US Army Center for Health Promotion and Preventive
Medicine – Depleted
Uranium.
- US Environmental Protection Agency, Office
of Pesticides Programs.
- US Environmental Protection Agency, Technology
Transfer Network, Hexamethylene-1-6-Diisocyanate.
|

