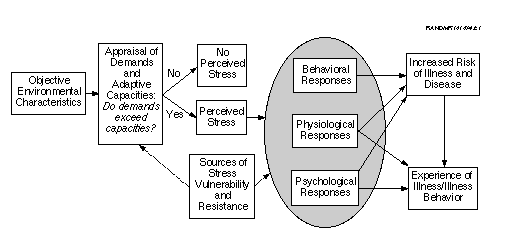
Figure 2.1--Conceptual Model Linking Stress Exposure to Poor Health
Thus, stress appraisals take into consideration an individual's repertoire of existing coping resources and individual vulnerabilities (Lazarus and Folkman, 1984; Kessler, Price, and Wortman, 1985; McEwen and Stellar, 1993; Steptoe, 1991), with these factors occupying a central role in most models of stress and health. Such models view stress as acting in concert with other factors to foster health problems, rarely regarding stress as a sufficient cause in itself. In fact, predisposing biological and psychosocial resources and vulnerability factors play a dual role in processes linking stress and health. First, individuals with more resources and fewer vulnerabilities may be less likely to perceive a given set of circumstances as stress-provoking. Second, when events are perceived as stressful, these individuals seem better able to adjust to the demands of the stress-provoking situation.[2] As shown in Figure 2.1, when sufficiently intense, perceived stress may activate physiological, behavioral, and psychological processes that place individuals at heightened risk for health problems or illness behavior (Cohen et al., 1995; Cohen and Rodriquez, 1995; Krantz et al., 1985; McEwen and Stellar, 1993; Steptoe, 1991).[3]

Figure 2.1--Conceptual Model Linking Stress Exposure to Poor Health
Most models suggest that physiological, behavioral, and psychological processes may directly influence health in specific ways. Physiological mechanisms implicated in illness and disease include the autonomic nervous system and neuroendocrine mediators that influence immune, gastrointestinal, neuromuscular, and cardiovascular systems among others (de la Torre, 1994; McEwen, 1998; McEwen and Stellar, 1993). Acute activation of these systems is known to precipitate short-term adaptive physiological changes as well as a whole range of somatic symptoms (e.g., rapid heart rate, increased perspiration, gastrointestinal motility) that may be experienced as symptomatic of ill health (Chrousos and Gold, 1992). Although physiological activation has short-term adaptive benefits, chronic activation of these systems is believed to enhance vulnerability to cardiovascular, metabolic, immune-related, and other diseases (Chrousos and Gold, 1992; McEwen, 1998; McEwen and Stellar, 1993) as well as changes in the central nervous system and the structure of the brain itself (Sapolsky, 1996). Recent evidence in both animals and humans also suggests that exposure to stressful events may increase the permeability of the blood brain barrier, thus rendering the central nervous system susceptible to drugs that typically act only on peripheral mechanisms (Friedman, Kaufer, Shemer, Hendler, Soreq, and Tur-Kaspa, 1996).
Behavioral responses to stress can also heighten risk of illness and disease. Individuals under stress are more likely to engage in behaviors with significant ramifications for health, including altered eating and sleeping habits and heavier consumption of alcohol and other substances (e.g., Brown, 1989; Conway, Vickers, Ward, and Rahe, 1981; McCann, Warnick, and Knopp, 1990).
Psychological mechanisms have been implicated as influencing health in at least two ways. First, patterns of thinking about oneself and one's world may place individuals at heightened risk for various forms of psychopathology, including depression (e.g., Beck, Rush, Shaw, and Emery, 1979) and anxiety (e.g., Schwarzer and Wicklund, 1991). Second, under stress, cognitive or social factors may heighten an individual's perception of himself or herself as sick, either by increasing awareness of bodily sensations that might otherwise go unrecognized (Pennebaker, 1982) or by prompting individuals to attribute normal symptoms or bodily sensations to evidence of pathology requiring medical intervention (Mechanic, 1972).
More recent research, using a taxonomy that distinguishes between high- and low-magnitude stressors, has systematically studied the possibility that war-zone deployment may be associated with a wide range of potential stressors (i.e., King, King, Gudanowski, and Vreven, 1995; Litz, King et al., 1997; Litz, Orsillo et al., 1997). These additional stressors include not only direct exposure to combat and other high-magnitude events such as exposure to atrocities (e.g., horrific carnage or body mutilation), but also to low-magnitude events such as separation from loved ones (Litz, Orsillo et al., 1997) and exposure to harsh living conditions such as lack of privacy, limited opportunity for recreation, long work hours, and difficult climatic conditions (King et al., 1995; Litz, King et al., 1997). Low-magnitude war zone stressors are not confined to separation from loved ones and harsh living conditions, however, and may include any other events or circumstances that foster a sense of personal disheartenment, discomfort, or demoralization (Litz, King et al., 1997).
The impact of war-zone exposure to low-intensity events has only recently been subjected to systematic empirical research (e.g., King et al., 1995; Litz, King et al., 1997), and much remains to be learned about the nature and circumstances in which these exposures lead to stress-related health consequences. Nonetheless, available data indicate that these seemingly ordinary experiences may be more potent stressors than previously believed. In particular, exposure to low-level daily hassles appears to predict adjustment outcomes independently of exposure to high-magnitude stressors. Consistent with general knowledge about stress exposure, recent empirical efforts to examine war-zone stress also underscore the importance of perceived, as well as actual, stressful circumstances (Solomon, Mikulincer, and Hobfoll, 1987; King, King et al., 1995). For example, analysis of data from the National Vietnam Veterans Readjustment Study (Kulka et al., 1990) revealed that self-appraised exposure to danger was a significant predictor of subsequent stress reactions (King, King et al., 1995).
In summary, a comprehensive representation of war zone stressors would consist of at least three components, any one of which may be sufficient to precipitate adverse stress reactions: (1) exposure to low-intensity events such as--but not limited to--harsh living conditions as well as separation from loved ones and its attendant hardships; (2) exposure to high-magnitude events such as involvement in actual combat or its often grotesque aftermath; and (3) exposure to conditions in which individuals perceive either themselves or others to be at risk of serious injury or loss of life.
[1]Laypeople commonly hold the misperception that mental and physical processes are unrelated to one another as manifested by the colloquial expression that stress is "all in the head." The roots of this fallacy can be traced to the mind-body distinction drawn by the early philosopher, Descartes, and run counter to current scientific knowledge (for discussion, see Damacio, 1994).
[2]Given the centrality of these factors that may heighten susceptibility or confer resistance to stress, they will be addressed in more detail in Chapters Four and Five.
[3]Most models regard illness and illness behavior as overlapping, but distinct, phenomena. Individuals may experience or perceive themselves as ill, thus stimulating illness behavior (e.g., medical help-seeking or staying in bed all day), even in the absence of any underlying syndrome (e.g., Mechanic, 1972; Pennebaker, 1982). Conversely, persons who are in poor health may not display illness behavior.